Bone Density Testing
Are you a woman age 65 years or older, a man age 70 years or older, or have you broken a bone (had a fracture) since age 50 years? If you answered “yes” to any of these questions, you should talk to your healthcare provider about getting a bone density test. Read on to learn about this, and more!
What Is a Bone Density Test?
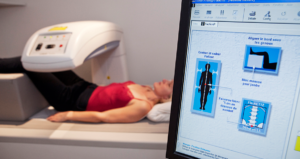
A bone density test is a measurement of how much mineral, such as calcium, you have in your bones. The most common and most versatile test is with dual-energy X-ray absorptiometry (DXA). This is used to diagnose osteoporosis BEFORE you break a bone, help to estimate your chances of breaking a bone in the future, and monitor the effectiveness of osteoporosis treatments. This is a very simple test that only takes a few minutes to do. You do not need to undress, but you must not have buttons or zippers in the area over your spine and hips. The test is non-invasive and painless; no needles or instruments are placed through the skin or body. There is very little radiation – far less than what you would get on a cross-country airplane flight. You simply lie on a DXA table and follow the instructions of the technologist to see that you are correctly positioned. Then a movable arm passes above you to scan your bones. Although this is very easy for you, the technology of the scan and computer system is actually very sophisticated. It requires highly trained staff to do the test properly and a qualified person to interpret it correctly. A good way to check on the qualifications of the person doing the DXA test is to ask whether they are certified by an organization such as the International Society for Clinical Densitometry (ISCD).
How Is Osteoporosis Diagnosed?
There are 3 ways that osteoporosis can be diagnosed. For each of these, confirmation of the diagnosis requires an evaluation to be sure there is no other disease or condition that appears to be osteoporosis but is not.
- Bone mineral density – The output of a DXA test is a number called a T-score. Normal is zero (0). The more negative the number, the weaker your bones and the more likely they are to break. If your T-score is -2.5 or below (such as -3.0), then you have osteoporosis, assuming there is no other reason for you to have such a low T-score.
- Fracture – If you are over the age of 50 years and have had a fracture of the spine, hip, wrist, humerus (shoulder), rib, and/or pelvis, then you probably have osteoporosis. A fracture of the spine or hip means osteoporosis regardless of your T-score. The occurrence of a fracture suggests that your bones are weaker than they should be and that further evaluation may be needed. In older adults, even fractures with major trauma, such as an auto accident, may be a sign of osteoporosis.
- FRAX – FRAX is a fracture risk calculator that is included in the software of most DXA systems and is accessible online for anyone at https://www.sheffield.ac.uk/FRAX/tool.aspx?country=9. With input of your bone density, your age, sex, height, weight, and answers to 7 questions, FRAX calculates the chances of you having different types of fractures in the next 10 years. If your 10-year probability of major osteoporotic fracture (meaning a fracture of the spine, hip, shoulder, or forearm) is 20% or more, or the 10-year probability of hip fracture is 3% or more, then a diagnosis of osteoporosis can be made.
Who Should Have a Bone Density Test?
Who should have a bone density test?
- Women age 65 years and older
- Men age 70 years and older
- Anyone who has broken a bone after age 50 years
- Women age 50-64 years with risk factors*
- Men age 50-69 years with risk factors*
*Examples of risk factors for osteoporosis and fractures include family history of osteoporosis and/or fracture, frequent falling, vitamin D deficiency, smoking, excessive alcohol intake, malabsorption, and some medications, such as prednisone.
Can DXA Do More Than Measure Bone Density?
DXA can be used to evaluate your bone health in ways that go beyond measuring bone density. Here are some of the other applications of DXA. These tests are available at some but not all DXA facilities.
- Vertebral fracture assessment (VFA) – This is a sideways image of the spine that can detect fractures, or crushed bones, in the spine. Most people who have these fractures do not know they are there. Identifying a previously unrecognized spine fracture may change your diagnosis, the estimation of your fracture risk, and treatment plans.
- Trabecular bone score (TBS) – This a number representing the internal structure of bones in your spine at the microscopic level. The higher the number, the better. It is generated with the use of special software added to the DXA system. The TBS number can be included in FRAX to give a better assessment of fracture risk.
Find Centers with TBS Osteo | Medimaps - Full-length femur imaging (FFI) – FFI is a technique for using DXA to get an image of your entire femur (thigh bone), instead of just the area around the hip that is seen with standard DXA. This can make it possible to recognize thickening of the bone that could lead to a stress fracture, or atypical femur fracture.
- Hip structural analysis (HSA) – The size, shape, and configuration of your hip bones can influence the strength of your hip and the likelihood of it breaking. HSA with DXA provides a way to look at this and may sometimes help with treatment decisions.
Are There Other Tests For Bone Density And Bone Health?
Many tests other than DXA can be used to assess your bone health. Some of them are not as widely used as DXA, but they may provide useful information beyond bone density, or help to determine who needs a DXA.
Quantitative Computed Tomography (QCT)
QCT provides a 3-dimensional measurement of bone density and can generate numbers that can be used to diagnose osteoporosis and for input with FRAX. Most types of QCT tests provide the same type of T-scores for bone mineral density at the hip as does DXA, but at the spine can provide a measurement of bone mineral density of just the spongy bone inside your vertebra. This type of spinal measurement may be preferred if your spinal bones have degenerative disease. QCT is not as widely used as DXA due to limited availability, higher radiation dose, and being less practical to monitor treatment for most patients.
Biomechanical Computed Tomography (BCT)
BCT is an advanced technology that uses data from a CT scan to measure bone mineral density. It is most commonly run on a CT scan you have already had or will have as part of clinical care for any reason as long as the scan includes an image of your hip and/or lower spine (for example an abdominal/pelvic CT scan to evaluate abdominal pain). BCT also uses engineering analysis (finite element analysis or FEA) to estimate bone strength (or measure the breaking strength of bone).
Radiofrequency Echographic Multi Spectrometry (REMS)
REMS is a portable method that does not use radiation that gives bone density measurements of the hip and spine.
Tests at Peripheral (Non-spine, non-hip) Sites
These types of tests measure bone density or other parameters in the peripheral skeleton, namely the arm, leg, wrist, fingers, or heel. Examples include:
- pDXA (peripheral dual energy x-ray absorptiometry)
- pQCT (peripheral quantitative computed tomography)
- QUS (quantitative ultrasound) – QUS, which is portable and uses no radiation, can be used to estimate fracture risk but cannot diagnose osteoporosis and is not useful to monitor treatment.
The results from these types of tests are not comparable to central DXA measurement and therefore difficult to interpret for diagnostic purposes and thus additional testing is often required. These types of tests serve mostly as screening tests to help identify people who are likely to benefit from further bone density testing at the hip and/or spine. Screening tests cannot accurately diagnose osteoporosis and should not be used to see how well an osteoporosis medicine is working.
- Pulse-echo ultrasound (P-EU) – uses no radiation and measures the thickness of cortical bone at peripheral skeletal sites with a handheld device. Studies have shown a significant correlation between measurements from P-EU and bone mineral density measured by DXA at the hip.
Where to Have a Bone Density Test
Most people need a prescription or referral from their healthcare provider to have a bone density test. If you’re not sure where to go for a bone density test, contact your healthcare provider or your insurance plan to find out where the test is available. The ideal facility is one with staff that are trained and certified by an organization such as the ISCD, and better yet, one that has been accredited by the ISCD. Most hospital radiology departments, private radiology groups, and some medical practices offer bone density testing. When you go for your appointment, be sure to take the prescription or referral with you. The testing center will send your bone density test results to your healthcare provider. You may want to make an appointment to discuss your results with your healthcare provider.
When to Repeat a Bone Density Test
As with any medical test, bone density should be repeated when the results might influence treatment plans. It is often repeated 1-2 years after starting or changing osteoporosis medication to evaluate response to treatment. It might also be repeated in 1-2 years if you are not being treated but are close to a treatment threshold. Subsequent testing varies according to your individual situation.
Understanding DXA Results
For postmenopausal women and men age 50 years and older, the T-score is the number that is used for diagnostic classification, as follows:
- A T-score of -1.0 or above is normal bone density. Examples are 0.9, 0 and -0.9.
- A T-score between -1.0 and -2.5 means you have low bone mass or osteopenia. Examples are T-scores of -1.1, -1.6 and -2.4.
- A T-score of -2.5 or below is a diagnosis of osteoporosis. Examples are T-scores of -2.6, -3.3 and -3.9.
It is important to recognize that you may be diagnosed with osteoporosis when the T-score is better than -2.5, as when you have already had a broken bone or FRAX shows that your risk is high. Also, when the T-score is 2-5 or below, you could have disease other than osteoporosis, such as osteomalacia or multiple myeloma. Your healthcare provider can evaluate you to be sure the diagnosis is correct or refer you to someone who can.
When to Consider Medications for Osteoporosis
The results of your bone density test, combined with all available clinical information, including your personal preference and previous experience with medications, can help with deciding to start, continue, or change medication to make your bones stronger and reduce the risk of breaking bones. Medications have been tested and approved for prevention and for treatment of osteoporosis. Each of these medications has its pros and cons. If you need take a medication, any one of them may be better than none, but some are better than others for increasing bone density and reducing the risk of breaking bones. Talk with your healthcare provider to find out which is best for you. If you decide not to take a medication, it is often a good idea to monitor your bone density and reconsider your treatment decisions from time to time. Regardless of whether you take a prescription medication, remember the essentials for good bone health: regular weight-bearing and muscle strengthening physical activity, maintaining good balance, avoiding falls, adequate intake of calcium and vitamin D, not smoking, avoiding excessive alcohol intake, and when possible, avoiding or minimizing exposure to drugs that are harmful to bones, such as prednisone.
Last Reviewed 3/8/2022